First person: Estos on the Front Lines - Tomas Saun
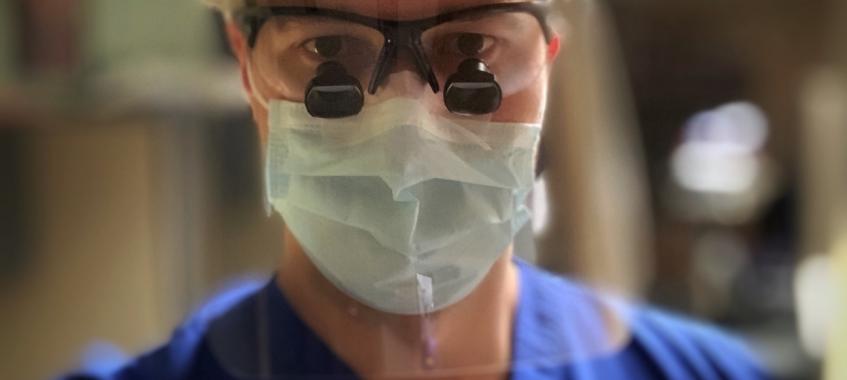
In 2018, Dr. Tomas Saun was an EFC Scholarship Recipient during his Masters of Applied Science in Biomedical Engineering. Today he is working on the front lines as surgical resident in Toronto. EFC asked him to share his experiences.
-------------------
My name is Dr. Tomas Saun, and I work at Toronto Western Hospital (TWH) as the Chief Resident, Hand and Wrist Surgery Service and am a Senior Resident, Plastic and Reconstructive Surgery at the University of Toronto.
During the Covid-19 crisis I have not been redeployed because the hand/wrist service at TWH has continued to see and operate on emergency patients throughout the pandemic. This includes mostly cases of hand/wrist trauma, broken bones, tendon/nerve injuries and replants (putting back on amputated fingers/hands). If anything it has become busier for me for two reasons: first, junior residents and medical students have been removed from our service and/or redeployed, and second we’ve been taking turns where only one resident comes in (normally 3-5 in every day) which means a lot of work for one person.
While I’m based at TWH during the day, when I'm on-call (which is typically every 3rd night or 10 nights out of 30 in a month) one plastic surgery resident covers multiple downtown hospitals including Toronto Western, Toronto General, Mount Sinai, Princess Margaret and Women’s College. In practice this often means running between hospitals to check on patients, see emergency consults, and operate. The other hospitals have also been active during the pandemic as cancer reconstruction cases have also continued.
Working during Covid
Overall, the hospitals have been very quiet as many wards are shut down and there are hospital-wide no visitor policies. When I’m here after hours I definitely feel completely alone – it’s very eerie at times. Our hospital has a face mask at all times policy, as well as eye protection/face shield at all times when seeing patients. All staff have to go through screening when entering the hospital.
For emergency surgery, because we don’t know the COVID status of patients, we have to ‘assume all patients are potentially covid positive’. This means that we have to wear N95 masks, and take extra precautions when seeing and operating on these patients. Also, anytime we use power tools in the Operating Room (such as drills and saws for bone surgery), we also have to wear special PPE as they are considered aerosol-generating. Some cases, such as when we are replanting fingers, can take 8-12 hours during which you’re wearing protective lead (for the xray) + gown + N95 mask + face shield -- which quickly becomes very uncomfortable. After these types of cases I usually am completely drenched in sweat and have skin tears on my face from the tape and adhesives
Since mid-march, there has been a complete shut down of all elective surgeries. This means that planned, nonemergency surgeries were not happening. I think this will have a major impact on my experience/education as I will be missing out on the practical experiences of these types of cases. As of this week, we’ve finally started a more regular operating room schedule. There are certainly a lot of additional challenges that the pandemic has created that I would’ve never anticipated when I started doing this 5 years ago, and I think this will change the way we practice forever, but I hope that we can get back to some sort of normal in the near future. But I still love my job.
PPE for Healthcare Professionals
We have definitely felt the effects of PPE shortage restrictions, but I don’t think I have ever felt like I did not have the appropriate PPE to do what I had to do. A lot of institutions have limited the learning opportunities for residents and other medical learners due to the PPE shortage (eg. They don’t want extra people around using the PPE if not absolutely necessary). Generally we are given one mask when we enter the hospital. We wear this until we get to our first clinical environment. Then we change for a new mask and face shield which we’re supposed to use for the rest of the day. In the operating room, we are given an N95 mask if the procedure is considered aerosol-generating or the patient’s covid status is unknown.
Tomas' Worries
At the start of the pandemic I definitely worried about contracting COVID myself and especially about bringing it back to my partner or my parents. I didn’t have contact with my parents for about 6 weeks during the initial outbreak. I was also definitely worried about being redeployed at the beginning. There was definitely a strong belief that most of us would be redeployed in some manner, but I haven’t worked in an ICU in many years, and I definitely worried that I didn’t have the skills/knowledge necessary to work in this setting. Having spoken with several residents/physicians who had/have been redeployed, however, they have all regarded it as a positive and rewarding experience and I’m sure I would’ve felt the same.
My partner and I were in isolation for the first 3 weeks of May because we tested positive for COVID. We were both completely asymptomatic and have had multiple negative tests afterwards. After coming back, I certainly feel a bit less worried as I hope I have established some immunity, but of course there is no certainty that you can’t get it again, or contract a variant.
One of my biggest concerns now is how this will impact my educational experience. I want to pursue fellowship training (extra training) in hand and wrist surgery when I’m done my residency and this rotation was pivotal in that pathway.
....and the future?
At work and society, I think we will see the repercussions of this for a long time. Things like physical and social distancing, plexiglass barriers, non-contact interactions will definitely persist. I think the response and outcomes of this pandemic will be critically evaluated and hopefully we can introduce more and better safeguards to protect us better if/when this happens again.
Want to know more? Read First Person:Estos on the Front Lines: Kristiina Nieländer-Hildebrandt - an ER nurse at Toronto Western Hospital or First Person: Estos on the Front Lines: Teija Jõgi - an acute care nurse at University Hospital in London, Ontario
TAKE ACTION
Donate
Sign Up
Get Involved
EFC
The Estonian Foundation of Canada is a registered charity that supports Estonian cultural and heritage initiatives across Canada.
Charitable No. 891452575 RR 0001
Contact
Google Maps
416.465.5600
E-mail Us




